What Causes Herpes Simplex Virus?
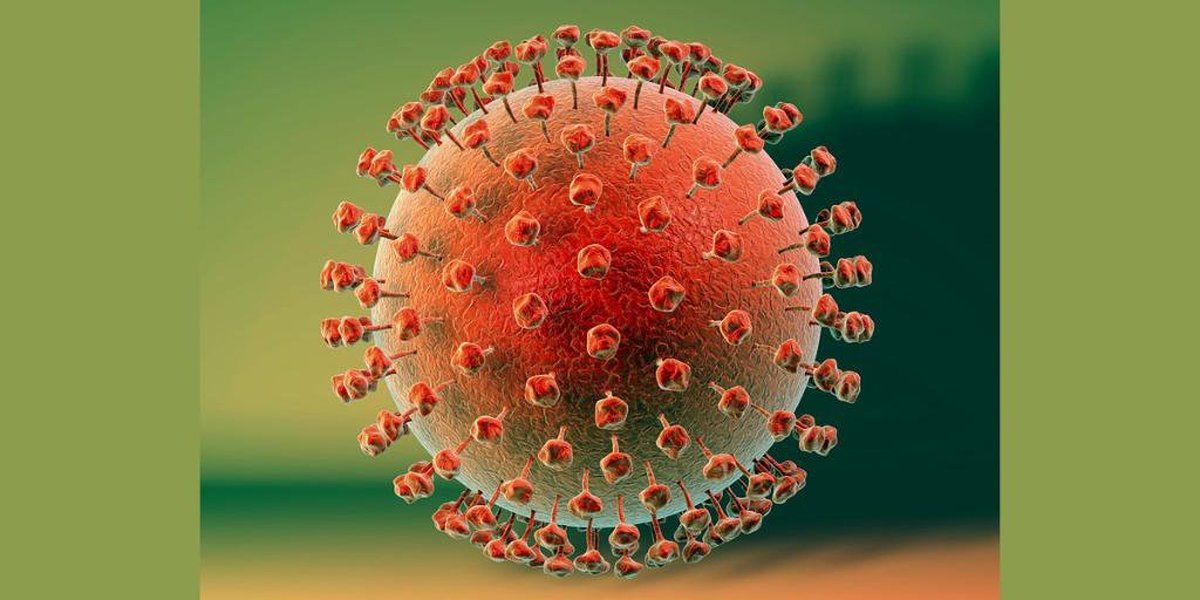
Herpes simplex virus (HSV) is caused by two closely related viruses: herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2). HSV-1 is mainly responsible for oral herpes infections around the mouth and lips which are also known as cold sores. HSV-2 causes genital herpes and infects the genital area, anus, buttocks or thighs. Both viruses are very contagious and spread through skin-to-skin contact with an infected region.
What Are The Symptoms of HSV?
The primary symptoms of an HSV infection include painful fluid-filled blisters or lesions in the infected areas around the mouth or genitals. These blisters ooze fluid and crust over to form small scabs. Other common symptoms include itching or tingling in the infected region before the appearance of blisters, pain during urination in case of genital infection, fever and swollen glands in the groin area. Recurrent infections may cause less severe symptoms or none at all. Asymptomatic shedding can also occur during which the virus is actively replicating without causing any visible symptoms.
Medical Treatments for Herpes Outbreaks
Both HSV-1 and Herpes Simplex Virus Treatment infections can be effectively managed through antiviral drug therapy. Some of the commonly prescribed oral antiviral medications for treating herpes outbreaks include:
Acyclovir (Zovirax): Acyclovir is a nucleoside analogue antiviral drug that interferes with the virus’s ability to replicate. It comes in topical and oral formulations for treating recurring cold sores and genital herpes.
Valacyclovir (Valtrex): Valacyclovir is a prodrug of acyclovir that gets quickly converted into active acyclovir in the body. Due to its higher bioavailability, it is more effective than acyclovir and is prescribed for suppressive therapy.
Famciclovir (Famvir): Like valacyclovir, famciclovir is also a prodrug of penciclovir which has antiviral activity against HSV viruses. It reduces healing time and symptom duration.
Pritelivir: This is a new generation antiviral drug approved to treat recurrent genital herpes. Unlike older drugs, it directly inhibits viral replication rather than depending on viral enzymes.
Medical interventions for HSV outbreaks also include topical creams containing numbing agents like lidocaine to alleviate pain from lesions. Antiseptic creams may help prevent secondary bacterial infections. Oral suppressive therapy is often recommended to reduce the frequency and severity of recurring infections.
Does Antiviral Therapy Provide A Cure?
While antiviral drugs provide effective symptomatic relief and mitigate outbreak severity, they do not cure HSV infection. This is because the virus has the ability to remain latent inside the body’s nerve cells without causing active symptoms. Even during latency, the virus is not completely eliminated from the body and reactivation occurs due to various triggers like stress, fatigue, skin trauma, UV exposure, immune suppression etc. Lifelong antiviral therapy aims to reduce symptomatic recurrences by keeping the virus in lifelong dormancy. A complete sterilizing cure still remains elusive for both HSV-1 and HSV-2. Researchers continue efforts to develop an HSV vaccine as well as novel antiviral strategies that could potentially cure herpes infections.
What Role Does The Immune System Play?
Our immune system plays a crucial role in preventing herpes reactivations and keeping the latency period symptom-free. Antibodies generated in response to primary HSV infection confer some degree of protection from recurring blisters by recognizing and eliminating the virus before it causes clinical disease. This explains why primary outbreaks tend to be more severe compared to subsequent milder recurrences in immunocompetent individuals. People with weak immunity like transplant patients on immunosuppressants are at much higher risk of frequent or severe herpes recurrences. Immune modulators or vaccines that boost HSV-specific immunity holds promise as an adjuvant treatment strategy along with antivirals.
Managing Stress and Daily Care
While medical intervention is important, self-care practices also help reduce symptomatic phases. Identifying and addressing psychological triggers like stress that may precipitate viral reactivation is recommended. Getting adequate sleep, managing daily stressors, consuming a balanced diet, staying hydrated and avoiding contact with known triggers are lifestyle tactics that bolster resistance towards recurrence. Keeping the infected area clean and applying hydrating creams provides comfort. Natural remedies with antiviral properties like lemon balm and licorice root may be useful as adjuvant therapies. Maintaining open communication with partners about sexual health can help prevent transmission. With proper medical management and self-care, herpes infections though lifelong can be effectively controlled.
In summary, despite being incurable herpes viruses causing recurring sores and lesions can be successfully managed long-term through a multipronged approach combining antiviral drugs, immune support, stress reduction techniques and preventive care practices. Addressing medical, psychological and lifestyle factors together optimizes control and minimizes symptomatic periods enabling those affected to lead fulfilling lives. Developing more advanced treatment strategies remains an ongoing endeavor that hopefully will yield complete sterilizing solutions in future.
*Note:
1. Source: Coherent Market Insights, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it.