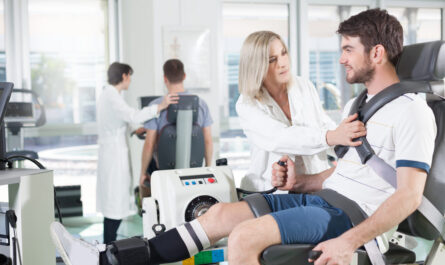
The medical devices reimbursement market deals with reimbursements for a variety of medical devices ranging from surgical devices, cardiac devices, orthopedic devices and many others that enhance patient care. Reimbursements enable patients to avail advanced medical treatments without significant financial burden.
Market Dynamics:
Reimbursements play a crucial role in enabling access to advanced medical treatments that rely on innovative medical devices. Two major drivers influencing the medical devices reimbursement market are:
First, mounting healthcare costs have prompted governments and private payers across countries to implement favorable reimbursement policies to enhance availability of newer medical technologies. This is expected to boost the market during the forecast period. Second, an aging global population vulnerable to complex health conditions will subsequently drive demand for state-of-the-art medical devices and fueled by adequate reimbursements. Furthermore, the need for cost-effective treatments is also propelling stakeholders to offer improved reimbursement schemes both nationally and internationally.
Aging Population is Driving Increased Demand for Medical Devices
The world’s population is aging rapidly as medical advancements allow people to live longer. This aging population is increasing the prevalence of chronic diseases that require long-term management with medical devices. Conditions like diabetes, heart disease, and arthritis become more common as people get older. As more people move into their golden years, demand will grow for devices that help manage and treat age-related illnesses. Population aging will propel governments and private insurers to expand reimbursement coverage and funding to support the growing need for medical technologies.
Rising Healthcare Costs are Pushing Governments to Tighten Reimbursement Policies
While an aging population drives more demand for healthcare services and technologies, skyrocketing costs threaten the sustainability of public reimbursement programs. The combined influences of medical inflation, more expensive treatments, and more beneficiaries are straining government budgets. To control unsustainable spending increases, policymakers are searching for ways to optimize the value received for reimbursement dollars spent. This could mean tightening eligibility guidelines, limiting coverage for certain products or procedures, standardizing reimbursement rates across care settings, or shifting more costs to consumers through higher co-payments and deductibles. The push to curb healthcare spending puts downward pressure on reimbursement in the medical device sector.
Opportunity for Value-Based Reimbursement Models
In response to rising healthcare costs, governments are experimenting with alternative reimbursement models that incentivize high-quality, cost-effective care over the volume of services. Value-based arrangements tie partial payment to providers achieving certain clinical outcomes or quality metrics, aligning incentives to focus on patient health rather than profit margins. This shift opens opportunities for medical device companies to demonstrate the long-term value and cost savings delivered by their products. Technologies supporting remote patient monitoring, fewer re-hospitalizations, improved adherence, and lower complication rates stand to benefit in a value-based environment. Medical device manufacturers have an incentive to prove return on investment through real-world evidence and value dossiers.
Move Towards Outcomes-Focused Reimbursement is a Growing Trend
Governments globally are transitioning away from traditional fee-for-service payment and towards increasingly outcomes-focused models. This recognises the need to optimize total cost of care and shift the emphasis from encounter-based services alone. Regulatory and policy changes now require demonstrating clinical effectiveness, quality of life improvements, economic benefits such as reduced hospital stays, and adherence to treatment protocols. Medical device companies must evolve beyond a product sale by improving health economics dossiers, data collection on real-world performance, and partnering with providers on risk-sharing contracts. Those able to quantify and prove value delivered across the continuum of care will gain competitive advantage amid tightening constraints and outcomes-oriented reforms to public reimbursement.
*Note:
1. Source: Coherent Market Insights, Public sources, Desk research
2. We have leveraged AI tools to mine information and compile it